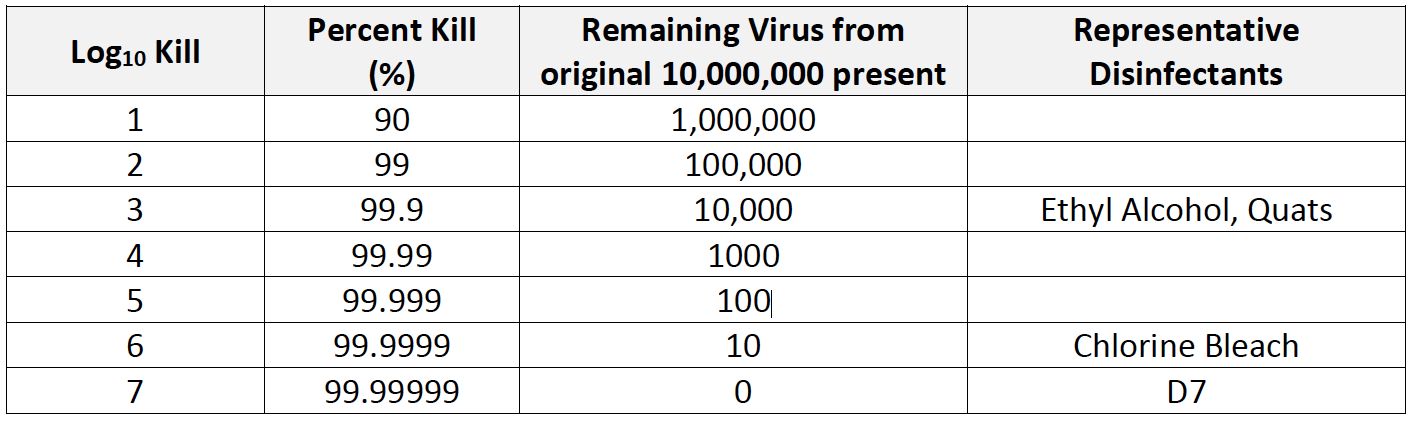
The second reason why D7 is a superior disinfectant for SARS-CoV-2 is that it has very high efficacy against a large spectrum of pathogens, including SARS-CoV-2. Efficacy in disinfectants is measured by log kill as shown in Table 1 below:
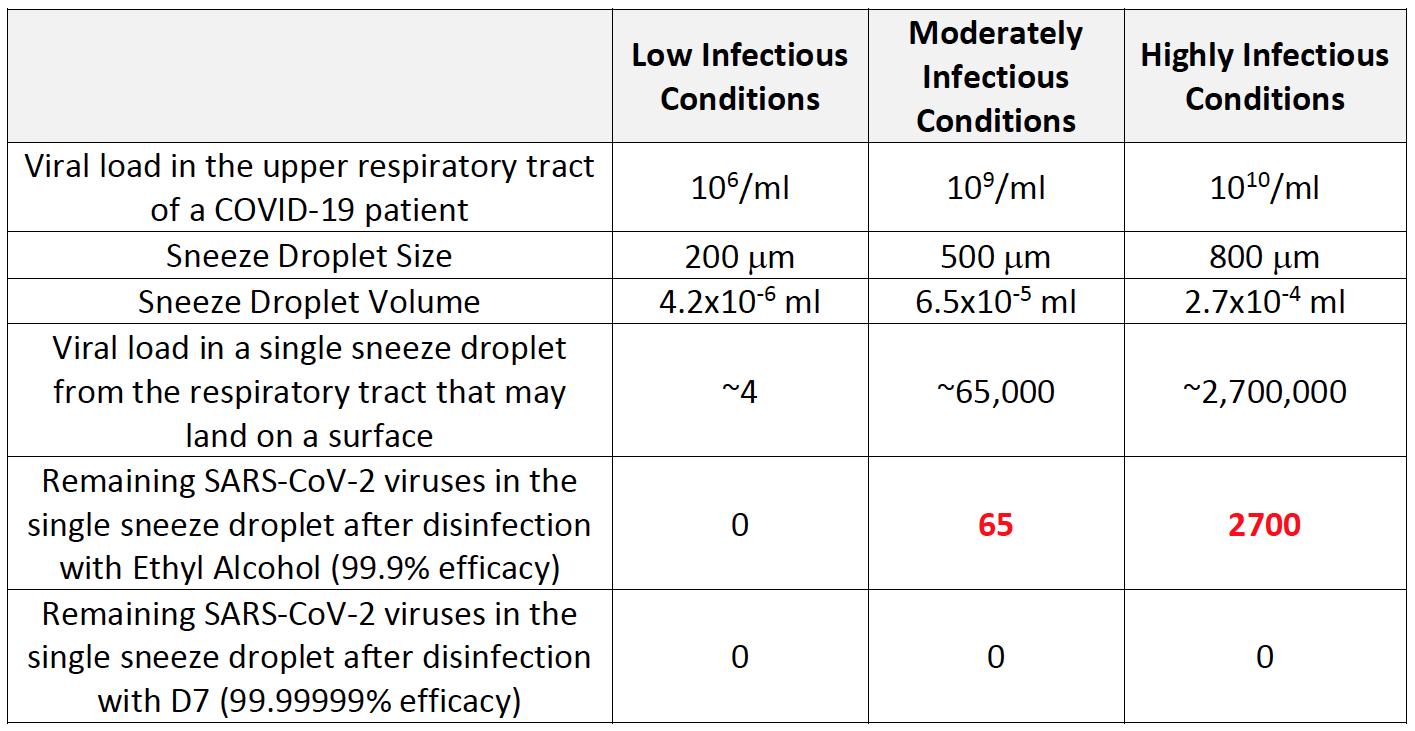
Unfortunately, many government organizations and others are promoting the use of low efficacy disinfectants in the battle against COVID-19. For example, most hand sanitizers use ethyl alcohol as their primary disinfecting ingredient. Other products may only contain a quaternary ammonium compound (i.e., quats) that also have relatively low efficacy. Using these types of disinfectants (and others with low efficacy) may present a significant problem because the large number of SARS-CoV-2 viruses deposited on a surface from the cough or a sneeze of an infected person may overwhelm these low efficacy disinfectants leaving infectious viruses behind even after disinfection operations. Recent research (Pan et al., Viral Load of SARS-CoV-2 in clinical samples, The Lancet, 20:4 [pp. 411-412], February 24, 2020) has shown that COVID-19 patients may have very high levels of SARS-CoV-2 viruses (i.e., viral load) in their upper respiratory system that could be expelled during a cough or sneeze. The sizes of a droplet expelled during a sneeze varies from <10 m to as large as 1000 m (Han et al., Characterizations of particle size distribution of the droplets exhaled by sneeze, Journal of the Royal Society, 10:88, November 6, 2013). Based on the data from these two studies, the number of SARS-CoV-2 viruses expelled during a sneeze from larger sized droplets (i.e., droplets that are likely to land on a surface) and the associated results of low efficacy vs. high efficacy disinfectants under various conditions (i.e., best case vs. worst case scenarios) are summarized in Table 2 below:
As can be seen, disinfection with low efficacy disinfectants (such as ethyl alcohol or quats alone) may leave infectious SARS-CoV-2 viruses on the surface which can lead to the possibility of new infections in people that come in contact with these surfaces or fomite transport (i.e., transport on shoes, clothing, equipment, etc.) to other surfaces and areas. The situation is likely worse than shown in Table 2 because, as noted above, ethyl alcohol type disinfectants may not even achieve their maximum efficacy because of the presence of bodily fluids and other organic matter. However, the situation is quite different if D7 is used because its higher efficacy can effectively destroy all the SARS-CoV-2 viruses in the sneeze droplets on the surface – even in highly infectious conditions.
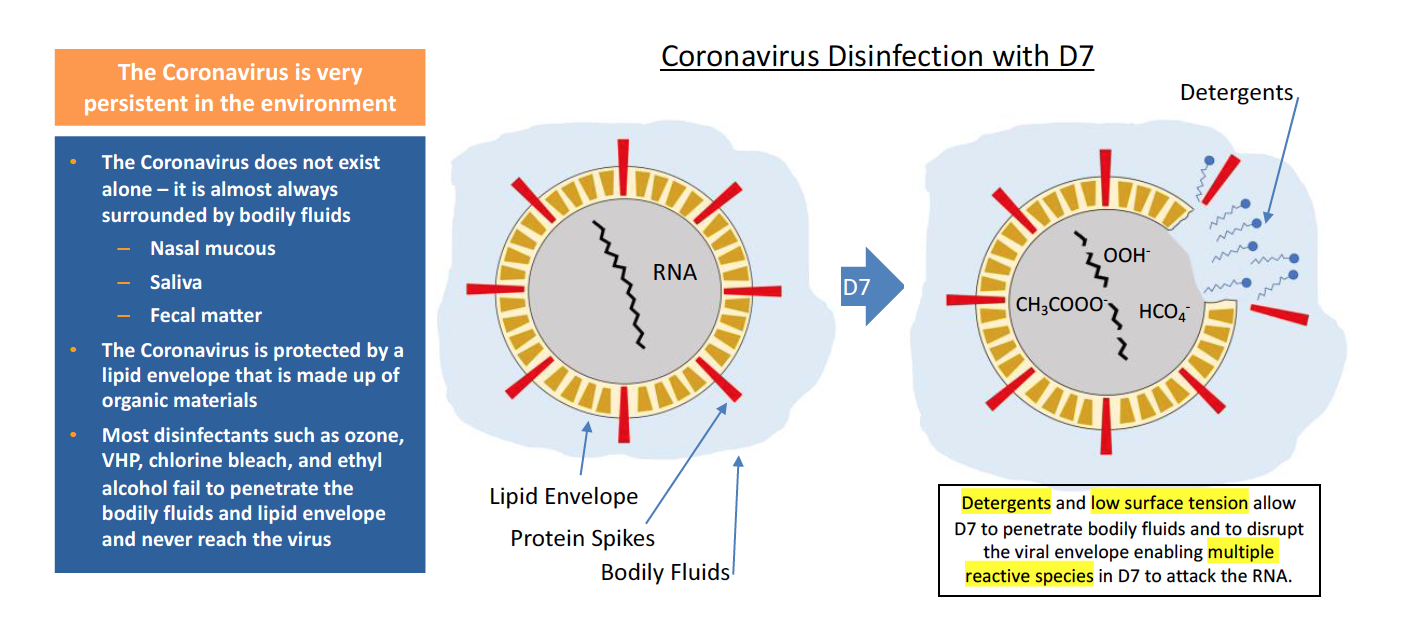
The final reason why D7 is so effective against SARS-CoV-2 is that it can easily be deployed by a variety of methods to handle any situation. It can be dispersed as a highly stable foam through existing foam generating equipment. When deployed as a foam, it clings to vertical and downward facing surfaces for 30 minutes or more to achieve long contact times against persistent toxic materials including biofilms. It can also be deployed as a liquid spray either through large-scale sprayers or from a hand-held spray can (i.e., BDAS+) which enables rapid deployment within seconds. D7 can also be deployed as a fog (or mist) from aerosol-generating devices primarily for interior decontamination – which is the ideal deployment method for both large and small spaces potentially contaminated with SARS-CoV-2. Finally, D7 can also be deployed by wetting microfiber towels and wiping touch points (e.g., door knobs, hand rails, escalator rails, etc.) where SARS-CoV-2 likely resides. Once D7 comes into contact with the virus, either in the air or on surfaces, it is quickly destroyed reducing the risk of infections to people in the area and reducing the potential for fomite transport. Most importantly, when D7 is deployed using any one of these methods, it eliminates SARS-CoV-2 even when it is embedded in soil, organic material, and bodily fluids which renders other disinfectants ineffective.